The opioid epidemic has profoundly affected communities nationwide, and college campuses are no exception. Rising rates of opioid misuse, coupled with the prevalence of fentanyl-laced substances, have amplified the risk of lethal overdoses among young adults. Around 50% of college sophomores report being offered an illicit opioid.¹ Additionally, a review of prescription opioid misuse among university students found lifetime misuse rates ranging from 4% to nearly 20%, with higher rates observed among students experiencing psychological distress, depression, or suicidal thoughts.²
Table 1. U.S. Drug Overdose Deaths by Category (2023)

Overdoses from stimulants like methamphetamine, cocaine, and ecstasy laced with opioids, often without the user’s knowledge, are increasingly common. In 2023, nearly 70% of stimulant-involved overdose deaths also involved fentanyl, highlighting the dangers of street drug contamination³. Cocaine-involved overdose deaths have quadrupled from 2015 to 2023, which is largely attributed to fentanyl contamination. These trends highlight a shift in the opioid crisis, where fentanyl, frequently undetected, now plays a deadly and growing role, especially on college campuses, where many students are exposed to illicit drugs.
The Michigan Emergency Medical Services Club (MEMSC) provides educational, volunteer, research, and career opportunities for students interested in healthcare and prehospital fields. MEMSC is a team of over 300 members, including 40 licensed EMTs. The development of this initiative was motivated in part by observations from students who work with the local ambulance service. Through their prehospital experience, several students noticed ambulance response times in the area can range from 10 to 15 minutes, depending on call volume and unit availability. In the event of an opioid overdose on campus, delayed ambulance arrival combined with the absence of readily available naloxone could allow respiratory depression to progress to cardiac arrest. These observations motivated students to address a critical window in which early bystander intervention with naloxone could be lifesaving.
Recognizing the growing public health challenge of opioid overdose, the Michigan Emergency Medical Services Club (MEMSC) launched a Naloxone Initiative to increase access to naloxone, a medication that rapidly reverses opioid overdoses. The Naloxone Initiative aims to install naloxone kits in fraternity and sorority houses, addressing the community’s elevated risk of substance use, and to empower students to intervene in opioid-related medical emergencies. The University of Michigan is home to 58 Greek Life organizations. We began the initiative focusing on both affiliated and non-affiliated Interfraternity Council (IFC) chapters and all affiliated Panhellenic Council (PHC) chapters. Our original focus did not include any professional organizations, as these groups are not part of the University of Michigan’s Fraternity and Sorority Life department, but reaching these communities would be a great next step for future expansion of our initiative.
The initiative followed a four-phase process of development: securing funding, forming relationships, education and training, and implementation. This article outlines the program’s development and offers recommendations for other collegiate EMS organizations looking to adopt similar harm reduction strategies.
Although the Naloxone Initiative was initially designed to serve fraternity and sorority communities, its structure can be adapted to other settings, including residence halls, student health centers, and off-campus housing. As opioid overdoses continue to affect various communities nationwide, increasing access to naloxone is a crucial step toward improving campus safety and preventing fatal overdoses.
Phase 1: Securing Funding
Michigan Emergency Medical Services Club is a Voluntary Student Organization (VSO) at the University of Michigan. VSOs apply for funding at the beginning of each semester through the Student Organization Funding Committee (SOFC), which is part of the Central Student Government. VSOs receive access to certain University-controlled benefits and resources, including funding, but are not directly sponsored by a university, school, or department. Grant applications are straightforward and request information about (1) the organization seeking funding, (2) specific information about the event, program, or service, (3) the anticipated impact on the student body, and (4) an itemized list of individual expenses.
Prior to requesting funding, we reached out to Wolverine Wellness, a health promotion program affiliated with the University of Michigan’s Student Health Services that supports student well-being. Wolverine Wellness regularly distributes free naloxone as part of its harm reduction efforts and agreed that providing the EMS club with naloxone for the project was feasible and aligned with their mission. Therefore, we acquired naloxone at no additional cost and anticipate being able to replace used or expired naloxone whenever needed.
We requested a total of $938 in funding for this project. All funding was allocated toward acquiring naloxone kits, which included the packaged naloxone as well as a case to hold the medication that would be installed in the chapter house. The grant proposal assumed all 58 chapters would agree to the installation of the kits. First, we determined that external weatherized outlet covers would serve as effective and accessible storage cases for naloxone kits. These are durable covers that snap shut and can be secured with breakaway ties. Installing the kits required screws and a drill. We recommend all of these materials to build effective kits, but acknowledge that financial costs will vary between agencies. We used a CPR-feedback mannequin, already owned by the club, to run a brief hands-only CPR demonstration, ensuring that trainees were prepared for an opioid-associated cardiac arrest.
Phase 2: Forming Relationships
Strong and collaborative relationships are a crucial part of this initiative. Gaining the support and participation of campus leaders and student organizations was essential to ensuring the initiative reached the communities most likely to benefit. We initially focused on a smaller and more feasible audience, with future expansion plans discussed later in this article to ensure naloxone education ultimately reaches all students and faculty.
Before engaging with our target audience, we formed relationships with key organizations on campus that could connect us with the resources we need. We were very fortunate that many University of Michigan programs, like LSA Student Government and Wolverine Wellness, were willing to provide a steady supply of naloxone to support our initiative. The University of Michigan Student Government also had its own programs dedicated to combating opioid overdose, so the relationships we formed with these student leaders led to an expansion of our initiative.
We identified five areas with potential gaps in access to naloxone where it could be of most value on a college campus: the Greek Life community, freshman residence halls, studenthealth centers, campus security vehicles, and anonymous pick- up stations. The identification of these five areas was informed by an informal needs assessment and environmental scan. We reviewed existing naloxone access points on campus to determine where naloxone was already readily available. Areas with established access, such as campus security, the emergency department, University Health Services, and an off-campus city library, were excluded from further consideration. Remaining areas were identified as potential gaps based on their high student presence, limited existing access to naloxone, and relevance to student safety.
Based on this assessment, our first target audience was the University of Michigan Greek Life community, specifically the IFC and PHC. We introduced the initiative in meetings with IFC and PHC leaders to gain approval and identify collaboration opportunities, and then communicated directly with chapter presidents. In these conversations, we outlined our goals and described how their chapters could participate, which included scheduling training sessions at chapter events to ensure all members received the education.
Entering the houses in person allowed us to build trust with the chapter leaders and members, and approach the sensitive topic of opioid overdose with compassion. Our goal was to promote a sense of shared responsibility and empower members of the Greek life community to make informed, safety-conscious choices. Some chapters were hesitant, raising concerns that the training might be uncomfortable, that naloxone’s presence could reflect poorly on their members, or that it might encourage opioid use. In response to these concerns, we refined our presentation to directly address these concerns and better meet the chapter where they were.
We included information about Michigan’s Good Samaritan Law, which protects individuals who provide medical assistance to someone experiencing an overdose from prosecution.⁴ We hope that this information encourages individuals to help those in need and relieve pressure associated with these high-stress situations. We also used familiar comparisons to training, such as CPR or fire extinguishers, which helped to emphasize that naloxone was simply another emergency preparedness tool that could help save a life. To make the presentation even more relatable and convincing to our audience, we included local statistics regarding overdoses from Washtenaw County, where Ann Arbor is located. Additionally, we provided contact information during every presentation so that members knew they could reach out with any questions or concerns. Lastly, we emphasized that the Michigan EMS Club does not pass judgment on anyone’s personal choices or social activities. Our sole aim is to provide objective information that may save lives and empower students to act in case of an emergency.
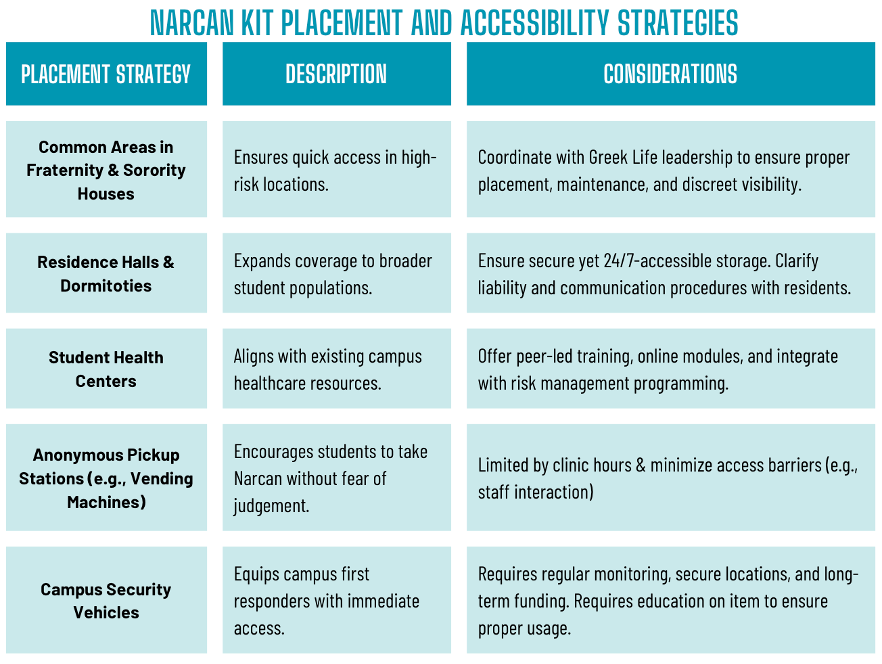
Table 2. Strategies for Naloxone Kit Placement and Accessibility on Campus
There is still ample work to be done in combating the opioid overdose problem, so maintaining long-lasting relationships is a priority for us. We will constantly be refining and updating this presentation as we connect with more communities to ensure we are always providing the most relevant and up-to- date information to participants. We also maintain contact with incoming chapter leaders during leadership transitions and promote our initiative amongst MEMSC club members to get younger members involved and ensure continuity of the initiative. We want to ensure our work is sustainable to educate and empower the ever growing community.
Phase 3: Education and Training
Simply placing naloxone in fraternity and sorority houses is not enough; students must feel confident in recognizing and responding to an opioid overdose for the initiative to be effective. The training material was developed to be concise and practical to avoid overwhelming participants while emphasizing the life-saving potential of naloxone.
Scheduling training sessions proved to be a logistical challenge, as chapters often had extensive existing social and philanthropic commitments. We found it most effective to offer training sessions during existing chapter events, rather than trying to coordinate separate sessions. This made participation more convenient, leading to greater attendance.
The Michigan EMS Club developed a 20-minute PowerPoint presentation with a hands-on skills session at the end. The in-person format allowed students to engage in demonstrations, ask questions, and receive direct feedback. The training covers three essential points: recognize the signs and symptoms of an opioid overdose, administer naloxone properly, and respond appropriately following administration. The curriculum was developed based on the Overdose Prevention and Response Toolkit, created by the Substance Abuse and Mental Health Services Administration (SAMHSA), a U.S. agency under the Department of Health and Human Services that addresses substance abuse and mental illness. The toolkit provides best practices recommended for responding to opioid overdose.⁵ Participants were taught to identify critical symptoms of a potentially fatal overdose, such as respiratory depression, loss of consciousness, cyanosis, and pinpoint pupils, and were instructed to call 911 immediately upon suspecting an overdose. Instruction on intranasal naloxone administration included positioning the individual supine, tilting the head back, inserting the device into either nostril, and firmly depressing the plunger. This demonstration was conducted using an empty naloxone nasal spray and a CPR mannequin.
The training emphasized the importance of updating 911 dispatchers on any changes in the patient’s condition following administration and guidance on what to do while waiting for first responders. By discussing the increasing prevalence of fentanyl-related overdoses, participants were encouraged to recognize that opioid overdose risk extends beyond individuals with a known history of opioid use.
Our team ensured that we acquired naloxone from dependable organizations to ensure that the supplies given to each chapter were safe and functional. Our discussion also points out several on-campus locations where students can obtain free naloxone, such as local fire stations and hospitals. We recommend that organizations implementing similar initiatives identify and share information about available supply hubs within their communities.
Discussions surrounding opioid overdose and naloxone can involve sensitive and high-risk scenarios; risk mitigation was a central consideration in training development. Our ultimate priority was to provide evidence-based information while clearly defining the limits of participant responsibility. Training content was reviewed by the Michigan EMS Club’s physician advisor to ensure appropriateness for a lay responder audience.
Participants were explicitly instructed that they should not enter unsafe environments to administer naloxone. Training reinforced legal protections for bystanders via Michigan’s Good Samaritan Law while emphasizing immediate activation of emergency medical services, underscoring that naloxone is an emergency tool and not a substitute for professional medical care. The entire scope of the education was intentionally focused on harm reduction and immediate emergency response; it strictly avoided teaching diagnostic guidance or advanced medical decision-making. Our organization worked with the University’s Central Student Government in implementing this program. Organizations seeking to replicate this model are encouraged to consult campus health services or institutional leadership as appropriate, based on local policies.
Phase 4: Implementation and Future Directions
After training is completed, each participating house is provided with two packaged doses of naloxone, ensuring a second dose is available if needed. We aimed to install the naloxone kits in the chapter house within a few days of the training. The naloxone is packaged in a clearly labeled storage container and is either mounted or placed in a secure location in the chapter house. Chapter leaders are responsible for sharing the location with all members. Additionally, some chapters have chosen to select specific members, deemed “sober monitors,” to carry the naloxone during social events.
For organizations that are interested in starting this work on their own campuses, but who do not have chapter houses, we recommend storing the naloxone in a safe, accessible place or assigning it to a responsible individual (e.g., a chapter president or risk manager) who can ensure its availability and communicate its location.
Our team conducts annual check-ins with chapters to offer a restock of any needed supplies and to gather updates on program implementation. During these check-ins, fraternity and sorority leaders are encouraged to share qualitative feedback on the program’s impact, including compliance with program protocols, any naloxone uses at chapter events, and remaining areas of need or support. Although a formal post-training survey was not administered during the initial implementation phase, we recommend that organizations seeking to replicate this model consider using structured surveys to evaluate participant confidence and preparedness.
We are excited about the future of our Naloxone Initiative. We aim to expand education and awareness surrounding this life-saving topic. We have been invited to collaborate with the IFC to include our presentation in New Member Orientation, an event for all individuals joining Greek Life to learn all about this new community, which will support us in reaching a broader audience within this high-risk group.
We also plan to expand the initiative beyond Greek Life. In collaboration with the University of Michigan’s Central Student Government (CSG), we are creating a website with comprehensive resources related to opioid overdose and naloxone. We intend to share this with the Greek Life community and other campus organizations to ensure widespread access to helpful and lifesaving information on opioid overdoses and safe naloxone usage. Ultimately, in partnership with CSG, we hope to incorporate naloxone training into the curriculum for the University of Michigan’s freshman orientation.
Conclusion
The Michigan EMS Club’s Naloxone Initiative is a proactive response to the growing opioid crisis. Grounded in community trust and public health best practices, the initiative has already resulted in the installation of naloxone kits in 10 sorority and fraternity homes. The EMS Club will continue implementation within the PHC and IFC community and expand outreach to other locations, such as residence halls and off-campus housing, to improve accessibility.
This article outlines the initiative’s development and challenges, and we hope that it serves as a guide for other collegiate EMS organizations looking to expand harm reduction efforts. We recognize each campus has its own structure and challenges, so we encourage flexibility when applying this model. More importantly, we hope this initiative inspires others to prioritize student health and safety. For questions, please contact us at umemsclub@gmail.com.
References
- Hedegaard H, Chen LH, Warner M. Drug-poisoning deaths involving heroin: United States, 2000–2013. NCHS Data Brief. 2015;(190):1-8.
- Weyandt LL, Gudmundsdottir BG, Holding EZ, et al. Prescription opioidmisuse among university students: a systematic review. J Am Coll Health. 2022;70(4):1119-1137. doi:10.1080/07448481.2020.1786095
- National Institute on Drug Abuse. Drug overdose deaths: facts and figures. National Institutes of Health. https://nida.nih.gov/research-topics/trends-statistics/overdose-death-rates
- SAFE Project. Good Samaritan Laws: State-by-State Analysis. SAFE Project. https://www.safeproject.us/good-samaritan-laws/
- Substance Abuse and Mental Health Services Administration. Overdose prevention and response toolkit. Publication No. PEP23-03-00-001. Published 2024. https://library.samhsa.gov/sites/default/files/overdose-prevention-response-kit-pep23-03-00-001
Acknowledgments
This initiative was made possible through funding provided by the University of Michigan Central Student Government’s Student Organization Funding Committee (SOFC). We gratefully acknowledge their financial support that enabled the purchase and installation of Narcan kits. We thank Wolverine Wellness for supplying naloxone kits and offering continued support for harm reduction efforts on campus. We also thank all of the University of Michigan students who participated in and contributed to this initiative. This project would not have been possible without them.
Author and Article Information
Noor Majhail, B.S., NREMT-P, graduated from the University of Michigan with a B.S. in Biology, Health, and Society and Spanish Language. She has served on the board of the Michigan Emergency Medical Services Club since 2022, previously as Vice President of Education and as Co-President (2024). Noor has led a variety of campus initiatives, including founding the UM Club Ambulance and teaching AHA BLS Provider courses, Hands-Only CPR, Stop the Bleed, and Narcan training sessions. Noor has been working in EMS for 4 years in Washtenaw County, MI. Sophie Raphael, B.S., NREMT-B, graduated from the University of Michigan with a B.S. in Biomolecular Science and a minor in Public Policy. Sophie has served on the Board of the Michigan Emergency Medical Services Club since 2022, previously as the Vice President of Community Outreach before assuming co- presidency in 2024. She has worked on a variety of campus initiatives, including CPR, Stop the Bleed, and Narcan training initiatives. Sophie has worked as an EMT for three years at home in Chicago, IL. Kate Metzendorf, B.A., NREMT-B, graduated from the University of Michigan with a B.A. in Sociology of Health and Medicine. She served as the Vice President of Operations for the Michigan Emergency Medical Services Club over the 2024-2025 academic year. In this role, she acted as director of the Narcan Initiative as well as managed the club’s Outreach Committee. Kate is a certified American Heart Association BLS Instructor and has taught multiple provider courses for University of Michigan students. She currently holds her New York State and National Registry EMT-B certification.




