
Introduction
Collegiate-based emergency medical services (CBEMS) are on-campus, student-run emergency medical services (EMS) organizations that respond to campus medical emergencies, supplement local emergency services, and offer health education to their communities. These organizations provide unique opportunities to improve response times, cultivate student leadership, and enhance campus safety.1,2,3,4 Despite their prevalence at over 250 colleges nationwide,5 such a program had not been successfully implemented in Washington state prior to the current initiative at the University of Washington (UW).
The founding team was composed of two first-year undergraduate Emergency Medical Technicians (EMTs) and a first-year medical student with CBEMS experience. The establishment of the UW Emergency Medical Services (UWEMS), a non-transport, Basic Life Support (BLS) agency, resulted as a culmination of focused advocacy efforts spanning from May 2023 to April 2025.
This manuscript provides a resource to future CBEMS agency founders by describing the genesis, development, and challenges related to the successful launch of UWEMS.
Understanding The Local System
The importance of a thorough understanding of the local EMS system and unique campus elements cannot be overstated. Differences in institution classification, size, and emergency response systems may influence how individual CBEMS agencies operate and, therefore, are established. The NCEMSF Startup Guide can serve as an excellent foundation,6 and founders should tailor the recommendations to the specific needs of their institution.
UW is a large, public, R1 institution with over 35,000 undergraduates and 15,000 graduate students.7 The Seattle Fire Department (SFD) leads the 9-1-1 response for both BLS and Advanced Life Support (ALS) emergencies on the UW campus. Most BLS transports are referred to a local private agency, American Medical Response (AMR), while Seattle Medic One handles ALS transports.8 Law enforcement support, when needed, is provided by the UW Police Department (UWPD) (Figure 1).
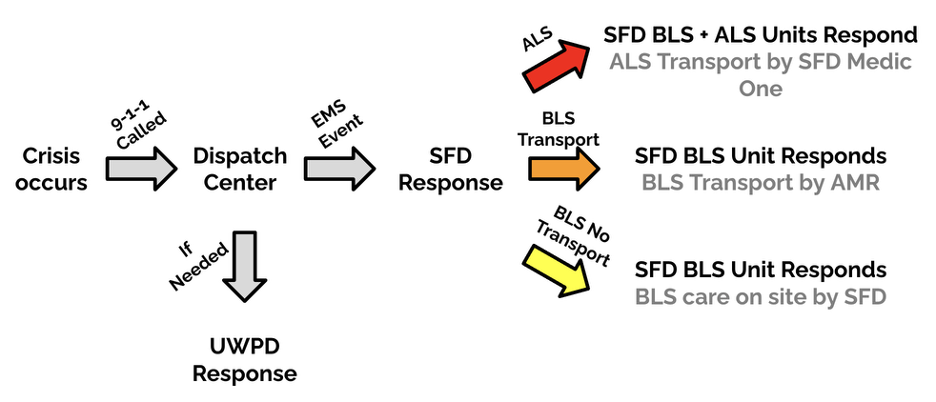
Figure 1. Response Model for On-Campus Emergencies at UW
Using historical data provided by SFDLive,9 a publicly accessible website logging all SFD responses, 468 medical responses to the university campus over the 2022-2023 academic year (July 1, 2022 – June 30, 2023) were analyzed. The mean response time was 6.6 minutes (standard deviation: 2.1 minutes). While this data is reflective of the unique challenges a large fire department would face in responding to a highly concentrated college campus, it highlighted an opportunity for improvement, as CBEMS agencies report a mean response time of 2.6 minutes (standard deviation: 1.7 minutes) due to their immediate proximity to the site of the emergency call.10
Laying a Strategic Foundation
The size of UW immediately limited the number of existing CBEMS models to which meaningful comparisons could be drawn. As such, the first priority was to identify true peer institutions and conduct interviews with their existing CBEMS agencies, emphasizing those founded more recently. This process resulted in relationships with a network of peer agencies who were regularly consulted throughout the implementation process.
Once the founding team could comfortably speak on the merits and practical applications of the CBEMS model, low-stakes conversations with community members were initiated. These individuals included a campus residence hall director, a physician at the on-campus clinic, and student government representatives. Through these discussions, the agency’s key characteristics were tailored to meet the unique elements of UW’s campus.
Drafting a Proposal and Vision
Creating a comprehensive proposal is the strongest way to communicate an agency’s goals and plan of action and can be instrumental to earning meetings and being taken seriously by important stakeholders. These included the Seattle Fire Department, the Central Region EMS & Trauma Care Council (CREMS),11 the UW, the WA Department of Health (WA DOH), and UW Medicine. In addition, a written document invited feedback from stakeholders in a manner that was productive and useful while respecting time constraints they may face during face-to-face meetings.
As most CBEMS founders are undergraduate students, demonstrating that the founding team is capable of understanding and proposing solutions to the challenges of CBEMS is essential in gaining trust and confidence from decision-makers. A detailed proposal can be critical in conveying this message. The final UWEMS proposal (see Appendix A) was highly detailed and descriptive. It relied on peer-reviewed literature alongside anecdotal information gathered from other CBEMS agencies. It included justification for the agency, an organizational chart (see Appendix B), a well-informed budget, a phased pilot program, mock shift schedules, a campus response zone (see Appendix C), a quality improvement plan, and liability coverage information.
Gaining Campus Support & Momentum
The most significant challenge faced by the founding team was converting casual intrigue in the mission of the program to truly committed campus support. Through conversations with university administrators, it was determined their reservations stemmed from five main barriers: a large financial burden, no third-party approvals, no political momentum, no liability strategy, and no administrative home (Figure 2).
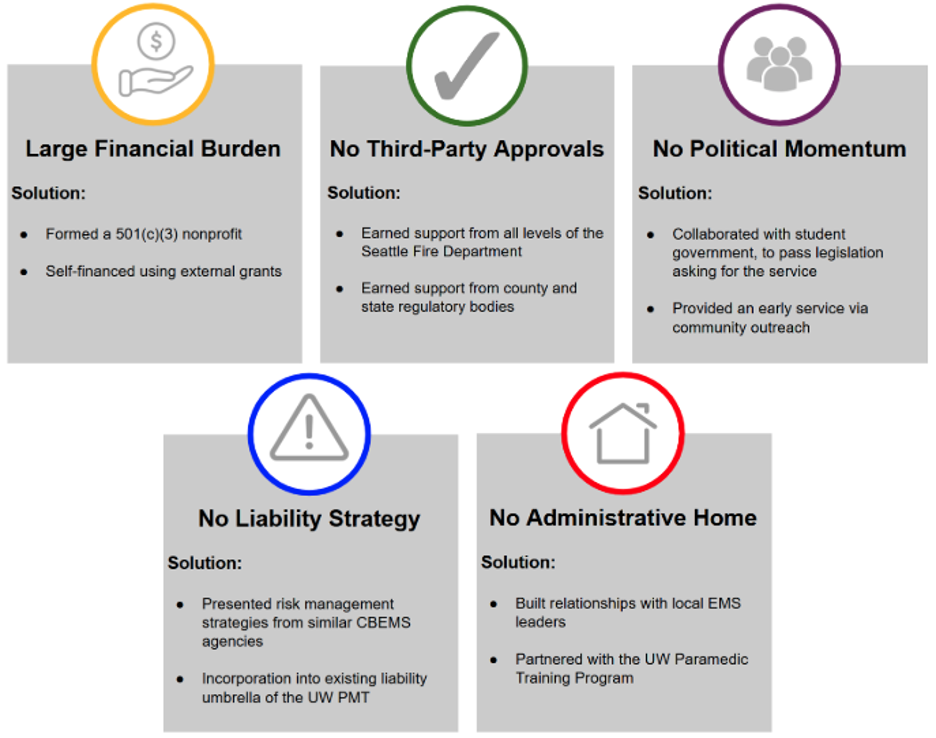
Figure 2: Summary of Barriers
Barrier 1: Large Financial Burden
One of the earliest challenges was to demonstrate the value of a CBEMS agency outweighed the financial risk, as stakeholders were hesitant to invest in a model that appeared costly and unproven. Requests for direct funding from multiple university departments were denied. In response, UWEMS was established as a 501(c)(3) nonprofit and fully financed through external grants and sponsorship to reduce institutional hesitancy and improve the overall risk profile.
Specifically, grants were secured through the Medic One Foundation, a non-profit focused on prehospital care in Northwestern Washington, a local private family foundation interested in promoting increased campus safety, and the CREMS. Additionally, a local bicycle company provided a discounted fleet of electric bicycles. Ultimately, over $60,000 in external funding was secured, enough to entirely finance the program launch and support at least 12-months of full-scale operation.
Barrier 2: No Third-Party Approvals
Early conversations with university administrators often stalled with the same concern: regardless of the new funding status, the proposal could not be considered without demonstrated support from external emergency response stakeholders. Namely, having the support of both SFD leadership and the Seattle Fire Fighters Union (International Association of Fire Fighters Local 27). Stakeholders across multiple levels of SFD’s chain of command were engaged, including the Captains at the local SFD station and the Fire Chief. Approaching these discussions by clarifying that UWEMS was intended as a complement to the existing response structure, rather than a replacement, proved important. These conversations also greatly helped in defining the scene of command procedures, scope of practice, and response logistics.
Building support from SFD Leadership and the Seattle Fire Fighters Union enabled further discussions with regulatory bodies including the WA DOH and CREMS. Strengthening these relationships early on provided greater leverage when reapproaching university departments.
Barrier 3: No Political Momentum
The founding team also needed to demonstrate that significant demand existed within the campus community for a CBEMS agency. This required strong community support from the campus at large. Consequently, legislation (Appendix D) was passed by the undergraduate student government supporting the establishment of UWEMS. Such approved resolutions are considered the official opinion of the entire undergraduate student body, which legitimized the need for a CBEMS agency. Once passed, the resolution was circulated amongst senior administrators, including the UW’s President and Provost.
At the community level, free CPR and naloxone training programs were launched, which served over 300 students in the first four months of operation. Providing an initial service to the campus, however small, showcased the potential of a CBEMS agency to fill campus needs and increased confidence in the program. In addition, the creation and staffing of these trainings helped build a pool of skilled, certified instructors who could also staff community events outside of UW to support external stakeholders.
Barrier 4: No Administrative Home
The founding team approached multiple departments within the university in an attempt to find an administrative home. While various UW stakeholders expressed support for the team’s mission, they all declined to serve in such a capacity, ultimately feeling they lacked the staff, infrastructure, or authority to provide ongoing oversight for a CBEMS agency. The founding team was frequently redirected to others, a reflection of the uncertain institutional path for integrating novel CBEMS programs.
Ultimately, the founding team was referred to the UW Paramedic Training Program (PMT) within the UW Medicine Department of Emergency Medicine as a potential administrative home. UW PMT holds the Emergency Services Supervisory Organization (ESSO) designation in Washington state and therefore has the legal capacity to adopt and oversee EMS agencies such as UWEMS.12,13 Their willingness to formally incorporate the agency and advocate for its inclusion from within the university ecosystem marked the key turning point in the agency’s trajectory.
The value of having a supportive administrative home and advisors within the university who could strongly advocate for the program cannot be overstated. In the case of UWEMS, these individuals were current and former physicians, paramedics, and nurses, who could draw from firsthand experience in EMS to assess and understand the vision while simultaneously balancing their understanding of the local emergency response ecosystem.
Barrier 5: No Liability Strategy
The final concern voiced by university administrators was the lack of a comprehensive liability strategy. Drawing from peer CBEMS agencies, a multi-model strategy was proposed to mitigate risk including independent emergency service insurance, mandatory liability waivers, and consultation with university legal counsel. Following incorporation with UW PMT, the Department of Emergency Medicine assessed the proposed strategies, and eventually elected to incorporate operations under its existing professional liability coverage and formally recognize UWEMS as a university-sanctioned emergency response program.
Implementing the Service
In order to become formally authorized to render care, an agency application was submitted to the WA DOH as an amendment to UW PMT ESSO. To ensure an adequate pool of qualified EMT candidates at the time of recruitment, interested students were directed to a local training program where they could complete their EMT certification. ‘Cohort 1’ was assembled by prioritizing first and second-year EMTs with external EMS experience and substantial alignment with the UWEMS mission. Recruits were quickly integrated into UWEMS operations and encouraged to take ownership of critical projects in preparation for launch.
The pilot program began with a structured rollout plan so UWEMS members and stakeholders could grow accustomed to how UWEMS would fit in the existing 9-1-1 response structure. The rollout plan included a preparatory phase, a shadowing phase, and a response phase. During the two-month preparatory phase, members were scheduled for informal, out-of-uniform shifts where they reported to headquarters and familiarized themselves with equipment and protocols without the pressure of active response. During the two-week shadowing phase, members began wearing uniforms and were dispatched to 9-1-1 calls, but did not enter the scene until SFD arrival, upon which they served as observers only. This allowed for practice with bike response, campus navigation, and the dispatch system. Finally, during the response phase, UWEMS assumed its intended operational scope, and members began initiating medical care upon arrival even if prior to SFD arrival on scene.
For the duration of the rollout plan, UWEMS scheduled its operational hours to coincide with periods of high campus 9-1-1 call volume. The stepwise rollout was a key component to success, as it allowed for the identification and rectification of pain points before they impacted full operations. In addition, it allowed time for the campus community to gain familiarity with the agency’s presence and scope.
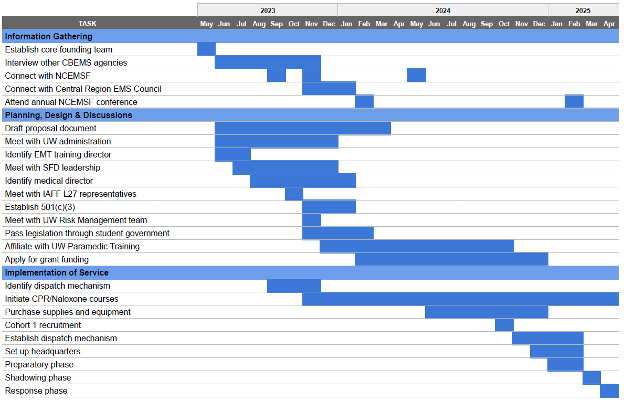
Figure 3. UWEMS 2023-2025 Timeline
Overcoming Setbacks & Challenges
With no precedent in Washington state, the concept of CBEMS was foreign to nearly all involved. Unforeseen challenges required numerous revisions to the original plans. Keeping the mission of UWEMS central to these changes allowed flexibility while maintaining forward momentum. For example, while the initial proposal included golf carts for campus response, logistical barriers like limited storage led to an electric bicycle model. Similarly, the proposed timeline for the pilot program shifted several times to accommodate unexpected delays and evolving circumstances.
Founding members of new CBEMS agencies should be prepared for a significant time commitment. It took over two years to get from idea formation to program launch. Early planning and a robust continuity of plans can help avoid disruption as founding members graduate before program launch.
Some of the greatest barriers involved navigating administrative obstacles, particularly in the first year of the founding process. These challenging discussions provided a better understanding of the priorities and concerns of various stakeholders and thus an opportunity to distinguish the proposed CBEMS agency from more traditional student groups. Here, the best approach was to remain patient, professional, and persistent in communications, always circling back to mission.
It is more than likely that founding teams will run into legal and regulatory hurdles unique to their states and universities. Both Washington state and the UW had no prior exposure to CBEMS. Interviewing and sharing resources with multiple CBEMS agencies across the country was incredibly helpful to the team in directing conversations and overcoming numerous hurdles.
Conclusion
On April 4, 2025, after over two years, UWEMS officially began providing patient care on the UW campus. From the start, the journey has been in firm conviction of the mission statement and the belief that students are capable, and sometimes best positioned, to create change. Leaning into the discomfort and unknowns that meet many CBEMS agencies, a program emerged that stands as one-of-a-kind in Washington state.
Acknowledgements
We would like to acknowledge the dozens of stakeholders, faculty, staff, advisors, and students who, without compensation, contributed to the formation of the agency. In particular, we would like to thank the University of Washington Paramedic Training Program for adopting UWEMS. We would also extend our gratitude to the members of the Seattle Fire Department and the National Collegiate Emergency Medical Services Foundation for their support. Finally, we thank our campus partners, including the Department of Emergency Medicine, UW Medicine, Associated Students of the University of Washington, Husky Health Center, University of Washington Police Department, Housing & Food Services, Division of Student Life, and Division of Campus Community Safety.
References
- Rosen JB, Olson MH, Kelly M. Collegiate-based emergency medical service: impact on alcohol-related emergency department transports at a small liberal arts college. J Am Coll Health. 2012;60(3):263-5.
- Friedman NMG, Koenig GJ, Marks JA, Hilton MT, Glick JE. Characteristics and outcomes of cardiac arrests reported in the national collegiate emergency medical services foundation data registry. J Am Coll Health. 2024;72(3):690-693.
- Jeffery RM, Dickinson L, Ng ND, DeGeorge LM, Nable JV. Naloxone administration for suspected opioid overdose: An expanded scope of practice by a basic life support collegiate-based emergency medical services agency. J Am Coll Health. 2017;65(3):212-216.
- Weber J, Potluri T, Chimata S, Dorosz E. More Than Just a Stepping Stone: The Lasting Legacy of Collegiate EMS Programs. JEMS. Published September 5, 2024.
- National Collegiate EMS Foundation. Home. NCEMSF. Published August 7, 2025.
- Grover J. Guide to Starting a Campus Based EMS Squad. Published December 2014.
- University of Washington. UW Fast Facts Pride Points 2024-2025. Published 2025.
- Seattle Fire Department. Medic One. Published 2019.
- Botello J. SFD Live: Seattle Fire Department real-time 911. Published 2025.
- Fisher J, Ray A, Savett SC, Milliron ME, Koenig GJ. Collegiate-based emergency medical services (EMS): a survey of EMS systems on college campuses. PDM. 2006;21(2):91-6.
- Reisenberg R. Central Region EMS & Trauma Care Council. Published 2025.
- Washington State Legislature. WAC 246-976-261: Emergency services supervisory organizations (ESSO). Published 2025.
- Washington State Legislature. RCW 18.73.030: Definitions. Published 2025.
Supplemental Materials
Appendix A:
Appendix B: UWEMS Organizational Chart
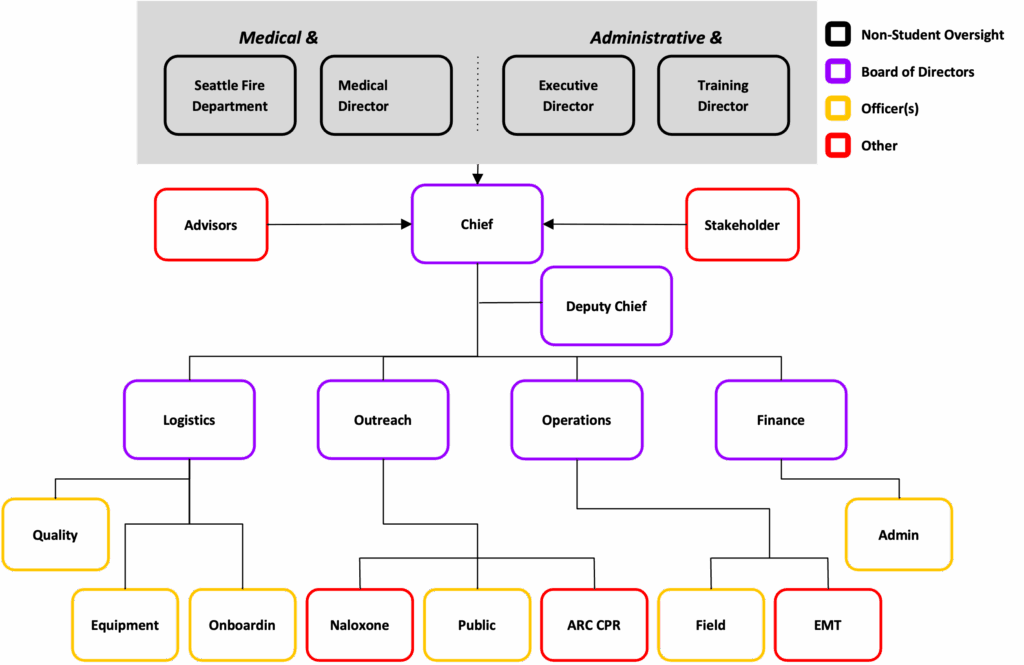
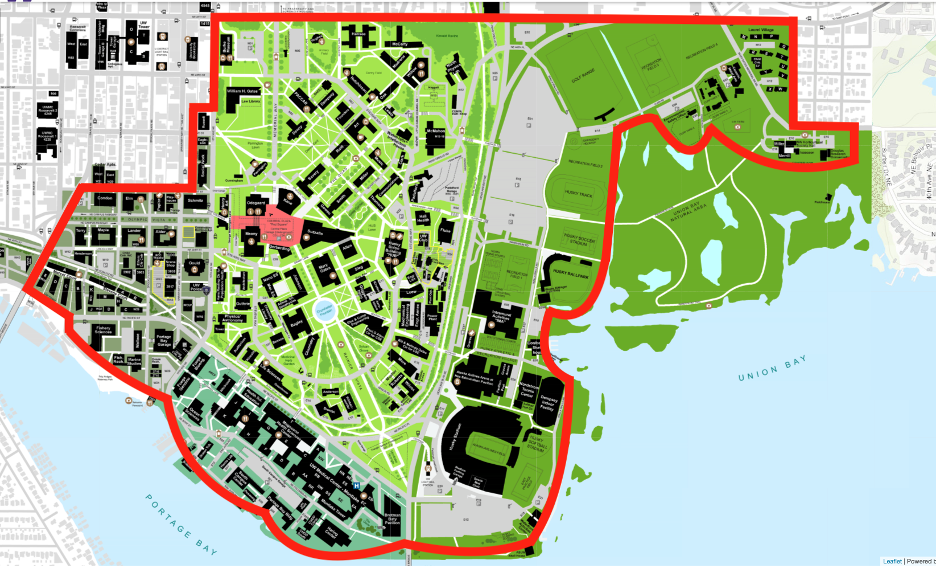
Appendix C: University of Washington Campus Map – UWEMS Response Zone
Appendix D: Board Bill 5.05 – Resolution for the Establishment of a Collegiate-Based EMS Program at University of Washington
Author & Article Information
Patrick Bi, BS, MBE, EMT is a third year medical student at the University of Washington School of Medicine, a founder of the University of Washington Emergency Medical Services, and holds a B.S. and Master’s in Biomedical Engineering from Rice University. Tristan Jafari, EMT is a senior earning a B.S. in Biochemistry at the University of Washington and a founder of the University of Washington Emergency Medical Services. Tanmay Bhanushali, EMT is a junior earning a B.S. in Linguistics at the University of Washington and a founder of the University of Washington Emergency Medical Services. Eric Timm, BSN, RN is the Director of the Paramedic Training program within the University of Washington Department of Emergency Medicine and Executive Director of the University of Washington Emergency Medical Services. Catherine R. Counts, PhD, MHA is an Assistant Professor within the University of Washington Department of Emergency Medicine Section of EMS
Author Affiliations: From University of Washington Emergency Medical Services – University of Washington – in Seattle, Washington (P.B., T.J., T.B., E.T.); University of Washington School of Medicine – in Seattle, Washington (P.B., E.T., C.C.)
Address for Correspondence: Patrick Bi | Email: bipatrick170@gmail.com
Conflicts of Interest/Funding Sources: By the JCEMS Submission Declaration Form, all authors are required to disclose all potential conflicts of interest and funding sources. By the JCEMS Submission Declaration Form, all authors are required to disclose all potential conflicts of interest and funding sources. All authors declared no conflicts of interest.
Authorship Criteria: By the JCEMS Submission Declaration Form, all authors are required to attest to meeting the four ICMJE.org authorship criteria: (1) Substantial contributions to the conception or design of the work; or the acquisition, analysis, or interpretation of data for the work; AND (2) Drafting the work or revising it critically for important intellectual content; AND (3) Final approval of the version to be published; AND (4) Agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Submission History: Received May 08, 2025; accepted for publication August 05, 2025
Published Online: August 31, 2025
Published in Print: Pending
Reviewer Information: In accordance with JCEMS editorial policy, Advice and Practice manuscripts are reviewed by the JCEMS Editorial Board and, as needed, independent reviewers. JCEMS thanks the Editorial Board members and independent reviewers who contributed to the review of this work.
Copyright: © 2025 Bi, Jafari, Bhanushali, Timm, & Counts. This is an open-access article distributed under the terms of the Creative Commons Attribution 4.0 International (CC BY 4.0) License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. The full license is available at: https://creativecommons.org/licenses/by/4.0/
Electronic Link: https://doi.org/10.30542/JCEMS.2026.08.01.04




